Does Your Patient Have an Underlying Peripheral Neuropathy?

You’ve been studying on the sofa with your leg tucked under you for the last hour. Now you’re ready to head to your kitchen for a quick snack, but your leg burns and tingles and your foot is numb. These symptoms occur because a nerve in your peripheral nervous system is compressed. Once the compression is removed from the nerve, the symptoms will soon disappear and you’ll be able to comfortably walk across the room.
Unfortunately, this is not the case for people with peripheral nerve problems. Neuropathy is a disorder that prevents the nerve from working properly, and if the root cause is not identified or addressed, the outcome may be chronic debilitating symptoms and overall functional decline.
Warning Signs and Early Symptoms
Peripheral neuropathy occurs when the sensory, motor, and autonomic functions of peripheral nerves are affected. Millions of people are diagnosed with peripheral neuropathy each year; however, the actual incidence is unknown as many people go undiagnosed.1
Early symptoms of peripheral neuropathy include pain, burning, loss of sensation, diminished tendon reflexes, weakness, and bone deformities. If autonomic nerves are affected, signs and symptoms may include alterations in heat tolerance and sweating, bowel or bladder problems, digestive problems, and changes in blood pressure. These symptoms can lead to subsequent problems such as skin breakdown, decreased balance, and overall decrease in movement.
One of the most common causes is diabetes mellitus, yet peripheral neuropathy can also result from traumatic injuries, infections, metabolic problems, inherited causes, and exposure to toxins.2 Common risk factors include:
- Specific diseases, including inflammatory (chronic inflammatory demyelinating polyneuropathy) or autoimmune diseases (lupus), infections (shingles), critical illnesses, and hereditary conditions (Charocot-Marie-Tooth disease)
- Environmental exposures, such as repetitive stressors
- Certain medications, such as chemotherapy, Dilantin, Cipro, or Levaquin
- Vitamin and nutritional deficiencies, such as a lack of B1 or B12
It is easy to see why the prevalence of peripheral neuropathy is so high while the condition remains difficult to detect at times. Complicating matters further, there are more than one hundred types of peripheral neuropathy, and each comes with its own set of symptoms and prognoses.3 In most cases, a good prognosis is dependent on early detection and individualized intervention.
Are You Screening for Peripheral Neuropathies?
Physical therapists play an important role in the early detection of peripheral nerve problems and can help patients improve and maintain function. Patients often present in the clinic with these symptoms and risk factors even when peripheral nerve involvement has yet to be identified. A neurological screening for peripheral nerve problems should be conducted for patients who present with diagnoses that may put them at risk.
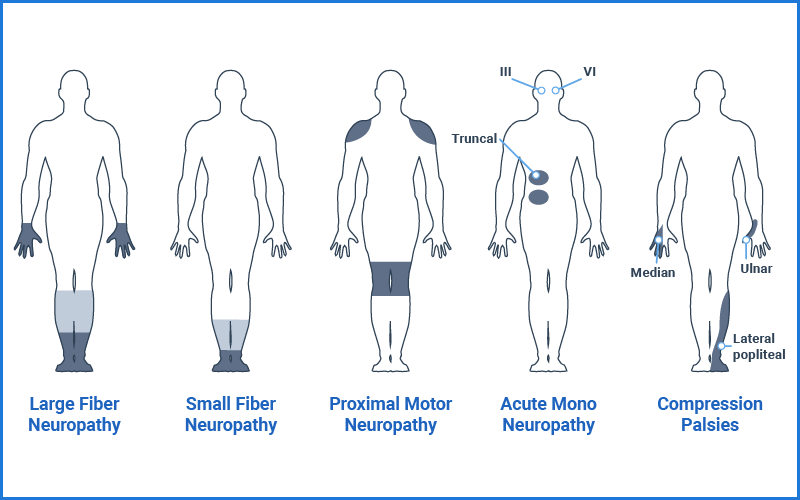
A full medical evaluation of peripheral neuropathy can be time-consuming and costly as it often includes a systematic approach using diagnostic imaging, electrodiagnostics, blood tests, and more. A simple neurological screen can help narrow down the possibilities and tailor the evaluation to a specific differential diagnosis while possibly reducing unnecessary testing.
Neurological screening should always include:
- Monofilament testing
- Vibration testing
- Deep tendon reflex (DTR) testing
The Essential Treatment List
Each patient’s treatment plan should depend entirely on the type of nerve damage and symptoms the individual person presents with. It should also address their unique diagnosis and risk factors. A comprehensive treatment plan coupled with patient-centered education may support functional recovery over time with little to no use of medications for some individuals. MedBridge’s Patient Education library includes nearly 400 patient-friendly, video-based resources, making it a great place to start.
Overall, each treatment plan should aim to:
- Improve patient/client knowledge and ability to self-manage pain
- Control inflammation
- Maintain or improve muscle length and flexibility
- Correct posture
- Improve muscle strength
- Improve movement quality
- Improve sensation
- Maintain nerve integrity
- Improve functional outcomes
- Improve overall health and fitness
What about Physical Agent Modalities?
Physical agent modalities represent a spectrum of adjunctive treatments therapists use to complement other therapeutic interventions and allow for a more comprehensive treatment plan.
Current evidence has shown:
- Transcutaneous electrical nerve stimulation (TENS) supports positive results for addressing pain and residual weakness.4, 5, 6
- Frequency rhythmic electrical modulation systems (FREMS) has promising results in the treatment of pain.7
- Long-standing and strong evidence supports neuromuscular electrical stimulation (NMES) for strengthening, volitional recruitment, and muscle reeducation in normally innervated but weak skeletal muscle.8, 9, 10, 11
- Electrical stimulation and low-level laser therapy have some encouraging evidence related to animal studies for nerve regeneration.12, 13, 14
Learn More about Managing Peripheral Neuropathies in Your Patients
In my MedBridge course, “Peripheral Neuropathies Part 2: Management of Common Presentations,” I review three types of peripheral neuropathies:
- Diabetic polyneuropathies—Peripheral nerves are damaged as a result of high blood sugar from diabetes mellitus. The most common type of neuropathy is chronic, length-dependent, and sensorimotor-focused.
- Guillain-Barré syndrome (GBS)—This autoimmune disease affects the peripheral nervous system. It is usually triggered by an acute bacterial or viral infection with resulting polyneuropathy.
- Bell’s palsy—This form of facial paralysis, most commonly an acute mononeuropathy, is due to damage or trauma of cranial nerve seven.
Expanding your knowledge so that you can easily identify, assess, and treat these three common neuropathies will allow you to offer your neurological patients a higher standard of care. Be sure to check out Part 1 of my series on Peripheral Neuropathies: “Peripheral Neuropathies Part 1: Diagnostics, Examination, and Treatment.” If you are considering specializing in neurological physical therapy and sitting for the NCS exam (or would simply like to build your expertise in this specialty), check out MedBridge’s NCS Prep Program, a highly focused study program that includes 50+ curated CE courses, recommended readings, 300 test items, and simulated examinations.
- National Institute of Neurological Disorders and Stroke. ( 2018). Peripheral neuropathy fact sheet. NIH Publication No. 18-NS-4853. Retrieved from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet
- The Foundation for Peripheral Neuropathy. (2016). Peripheral neuropathy risk factors + facts. Retrieved from https://www.foundationforpn.org/what-is-peripheral-neuropathy/types-risk-factors/
- Johns Hopkins Medicine. (n/d). Peripheral neuropathy. Retrieved from https://www.hopkinsmedicine.org/healthlibrary/conditions/nervous_system_disorders/peripheral_neuropathy_134,51
- Dubinsky, R. M. & Miyasaki J. (2010). Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology, 74:173-176.
- Fuentes J., Olivo, S., Magee, D., & Gross, D. (2010). Effectiveness of interferential current therapy in the management of musculoskeletal pain: a systematic review and meta-analysis. Physical Therapy, 90(9):1219–1238.
- Kılınç, M., Livanelioğlu, A., Yıldırım, S. A., & Tan, E. (2014). Effects of transcutaneous electrical nerve stimulation in patients with peripheral and central neuropathic pain. Journal of Rehabilitation Medicine, 46(5): 454-460.
- Bosi, E., Bax, G. Scionti, L., Spallone, V., Tesfaye, S., Valensi, P., & Ziegler, D. (2013). Frequency-modulated electromagnetic neural stimulation (FREMS) as a treatment for symptomatic diabetic neuropathy: results from a double-blind, randomised, multicentre, long-term, placebo-controlled clinical trial. Diabetologia, 56(3): 467-475.
- Gordon, T. & English, A. W. (2016). Strategies to promote peripheral nerve regeneration: electrical stimulation and/or exercise. The European Journal of Neuroscience, 43(3): 336-50.
- Asensio-Pinella, E., Udina, E., Jaramillo, J., & Navarro, X. (2009). Electrical stimulation combined with exercise increase axonal regeneration after peripheral nerve injury. Experimental Neurology, 219(1): 258-265.
- Gordon, T. (2016). Electrical stimulation to enhance axon regeneration after peripheral nerve injuries in animal models and humans. Neurotherapeutics, 13(2): 295-310.
- Sheffler, L. R. & Chae, J. (2007). Neuromuscular electrical stimulation in neurorehabilitation. Muscle & Nerve, 35(5): 562-90.
- Barbosa, R. I., Marcolino, A. M., de Jesus Guirro, R. R., Mazzer, N., Barbieri, C. H., & Fonseca, M. d. C. R. (2010). Comparative effects of wavelengths of low-power laser in regeneration of sciatic nerve in rats following crushing lesion. Lasers in Medical Science, 25(3): 423-430.
- Mandelbaum-Livnat, M. M., Almog, M., Nissan, M., Loeb, E., Shapira, Y., & Rochkind, S. (2016). Photomedicine and Laser Surgery, 34(12): 638-645. Rochkind, S., Drory, V., Alon, M., Nissan, M., & Ouaknine, G. E. (2007). Laser phototherapy (780 nm), a new modality in treatment of long-term incomplete peripheral nerve injury: a randomized double-blind placebo-controlled study. Photomedicine and Laser Surgery, 25(5): 436-42.









