Optimizing Complex Cases in Joint Arthroplasty
Presented by John O’Halloran
12-Month Subscription
Unlimited access to:
- Thousands of CE Courses
- Patient Education
- Home Exercise Program
- And more
Achieving superior clinical results after joint replacement requires moving beyond standard protocols to address patients who have not achieved normative surgical expectations. While joint arthroplasty is generally successful, approximately 20% of knee patients remain dissatisfied, and many hip patients continue to experience persistent gait abnormalities and increased fall risks. This course provides a comprehensive troubleshooting framework for identifying the underlying causes of chronic pain, stiffness, and mechanical dysfunction in the shoulder, hip, and knee. Participants will master advanced motor control strategies and manual therapy techniques, such as short-lever deltoid facilitation and lumbopelvic corrective exercises, to resolve complex issues, such as the “shoulder shrug” and pelvic asymmetry. Designed for physical therapists and healthcare providers in outpatient settings, this curriculum offers evidence-based solutions for the most challenging postoperative cases, ensuring every patient returns to a high level of function.
Learning Objectives
- Analyze the underlying factors that lead total shoulder arthroplasty patients to develop compensatory shoulder hike or shrug patterns
- Select appropriate motor-control treatment strategies to promote a faster and more normalized gait pattern following knee and hip arthroplasty
- Deduce sources of pain in total hip and knee patients by identifying probable contributing factors
- Implement manual therapy and corrective exercise interventions to address stiffness in total knee arthroplasty patients
- Integrate corrective exercise strategies to reduce fall risk in individuals following total hip or total knee arthroplasty
Meet your instructor

John O’Halloran
John O’Halloran, PT, DPT, OCS, ATC (retired), CSCS (retired), Cert MDT, Certified SCTM-1 Practitioner, is a board-certified orthopedic clinical specialist by the American Physical Therapy Association with over 30 years of experience in the field of orthopedics. He earned his postprofessional Doctor of Physical Therapy from…
Chapters & learning objectives

1. The Shoulder Hike or Shoulder Shrug Arthroplasty Patient
This chapter investigates the underlying problems and predisposing factors that lead to compensatory shoulder shrugging or hiking following shoulder arthroplasty. Clinicians will learn to implement kinetic link rehabilitation and short-lever-arm deltoid facilitation to improve the functional range of motion in patients with rotator cuff deficiency.

2. Altered Gait in the Total Hip and Knee Patient
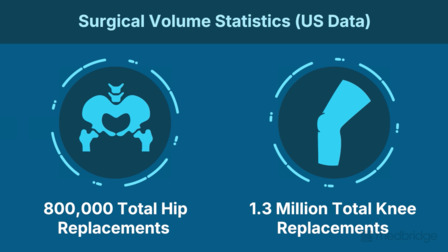
Participants will analyze statistical data on patient dissatisfaction and identify the determinants of persistent gait compensation and postsurgical fall risk. This section provides practical tips for addressing leg length discrepancies caused by pelvic asymmetry and strategies to facilitate terminal hip extension to normalize stride length.

3. The Stiff Total Knee Patient
This chapter explores the primary causes of chronic stiffness after total knee replacement, including arthrofibrosis, implant malalignment, and the impact of revision surgery. Clinicians will examine current research on range-of-motion recovery after 12 weeks and master manual therapy techniques to improve mobility in challenging cases.

4. The Painful Hip and Knee Patient
Clinicians will learn to deduce the source of chronic pain by identifying probable causes such as low-grade infection, metal sensitivities, and active trigger points. This section highlights specific clinical conditions, such as neuromas and anterior knee pain, while evaluating the safety and efficacy of genicular nerve radiofrequency ablation.
More courses in this series

Optimizing Outcomes After Total Joint Arthroplasty
John O’Halloran
Optimizing Function After Shoulder Arthroplasty
John O’Halloran
Optimizing Gait After Hip Arthroplasty
John O’Halloran
Optimizing Recovery After Knee Arthroplasty
John O’Halloran
Optimizing Complex Cases in Joint Arthroplasty
John O’Halloran