Optimizing Outcomes After Total Joint Arthroplasty
Presented by John O’Halloran
12-Month Subscription
Unlimited access to:
- Thousands of CE Courses
- Patient Education
- Home Exercise Program
- And more
Modern surgical advancements have radically shifted the landscape of joint replacement, moving from week-long hospital stays to a reality where over 75% of cases may soon be same-day surgeries. Despite these technological leaps, a significant gap remains in postoperative satisfaction, as approximately 26% of total knee patients report being less than satisfied one year after their procedure. This course addresses this clinical disconnect by exploring the critical recovery window and the necessity of shifting from “mindless rehab” to high-level clinical decision-making. Participants will evaluate contemporary technologies such as robotic-assisted surgery and smart implants while mastering practical strategies for prehabilitation and the early facilitation of functional gait. Designed for physical therapists and healthcare providers across acute care, home health, and outpatient settings, this course provides the tools to mitigate persistent impairments and improve long-term patient-reported outcomes.
Learning Objectives
- Analyze the history of joint replacement and the advanced technologies used in contemporary arthroplasty
- Examine key facts and figures related to joint replacement, including factors associated with patient dissatisfaction
- Determine why prehabilitation and the first 21 days after joint replacement are critical to successful recovery
- Distinguish rehabilitation approaches across acute care, skilled nursing, home health, and outpatient settings
- Integrate bed exercises, core training, and functional weight-bearing activities into early postoperative rehabilitation following joint arthroplasty
- Categorize gait cycle characteristics and research-identified gait compensation patterns, along with the postoperative impairments that commonly persist after hip and knee arthroplasty
Meet your instructor

John O’Halloran
John O’Halloran, PT, DPT, OCS, ATC (retired), CSCS (retired), Cert MDT, Certified SCTM-1 Practitioner, is a board-certified orthopedic clinical specialist by the American Physical Therapy Association with over 30 years of experience in the field of orthopedics. He earned his postprofessional Doctor of Physical Therapy from…
Chapters & learning objectives

1. Trends in Joint Replacement
This chapter examines the historical progression of joint replacement and the cutting-edge technological advancements, such as robotic-assisted surgery and 3D-printed implants, that define contemporary practice. Understanding these surgical innovations is essential for providers to align rehabilitation goals with the specific capabilities and limitations of modern prosthetic designs.

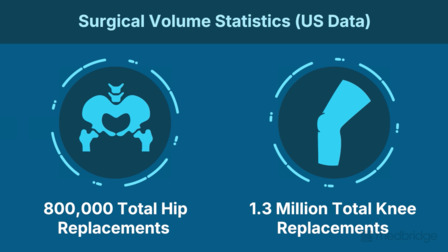
2. An Aging Population
As joint replacements transition toward same-day discharge and an aging demographic, clinicians must understand the impact of new reimbursement models and shifting patient expectations. This section highlights factors contributing to patient dissatisfaction and the rising demand for revision surgeries, emphasizing why therapists must adapt to a more efficient, evidence-based care delivery model.

3. Arthritis and the Joint
This chapter explores the global impact of osteoarthritis as a leading cause of disability and evaluates the various conservative management strategies used before surgical intervention. Clinicians will examine the role of injections, bracing, and activity modification, as well as how these factors influence the eventual timing and success of a total joint arthroplasty.

4. Improved Outcomes
Clinicians will analyze the critical role of prehabilitation and perioperative pain management in securing successful long-term outcomes and reducing hospital stays. By addressing inclusion and exclusion criteria for outpatient surgery, providers can better manage patient expectations and identify those at risk for persistent postoperative impairments.

5. Postoperative Exercises
This chapter provides actionable techniques for the early facilitation of function, including core integration and specific exercises to regain terminal joint extension. Moving beyond basic protocols, participants will learn to optimize the kinetic chain and functional gait patterns to ensure patients return to their highest level of activity.
More courses in this series

Optimizing Outcomes After Total Joint Arthroplasty
John O’Halloran
Optimizing Function After Shoulder Arthroplasty
John O’Halloran
Optimizing Gait After Hip Arthroplasty
John O’Halloran
Optimizing Recovery After Knee Arthroplasty
John O’Halloran
Optimizing Complex Cases in Joint Arthroplasty
John O’Halloran