Optimizing Function After Shoulder Arthroplasty
Presented by John O’Halloran
12-Month Subscription
Unlimited access to:
- Thousands of CE Courses
- Patient Education
- Home Exercise Program
- And more
Advanced surgical techniques and multimodal pain management have revolutionized shoulder reconstruction, yet achieving optimal functional outcomes remains a complex clinical challenge. This course addresses the critical shift toward same-day surgery and the specific rehabilitation strategies required to manage the rising volume of both anatomic and reverse shoulder replacements. Participants will examine the biomechanical nuances of various shoulder prostheses, including the emergence of reverse total shoulder arthroplasty (rTSA) for patients with rotator cuff deficiency. Through an evidence-based lens, the curriculum explores manual techniques, soft-tissue releases, and short-lever exercises designed to facilitate deltoid function and restore above-average range of motion. Designed for physical therapists and healthcare providers in outpatient and home health settings, this course provides a comprehensive framework for navigating the recovery phases and managing patient expectations for a successful return to sport and daily activity.
Learning Objectives
- Analyze the history of shoulder arthroplasty, including the evolution of surgical procedures
- Categorize the rehabilitation phases for shoulder arthroplasty and the expected ranges of motion associated with each phase
- Implement manual therapy strategies—such as fascial release—to promote functional range of motion beyond normative levels
- Prepare therapeutic exercise progressions, with an emphasis on short-lever-arm, deltoid-assisted variations
- Determine postoperative expectations for return to functional activity and participation in daily activities
- Distinguish the phases of rehabilitation following reverse total shoulder arthroplasty and the factors contributing to the recent rise in procedure volume
Meet your instructor

John O’Halloran
John O’Halloran, PT, DPT, OCS, ATC (retired), CSCS (retired), Cert MDT, Certified SCTM-1 Practitioner, is a board-certified orthopedic clinical specialist by the American Physical Therapy Association with over 30 years of experience in the field of orthopedics. He earned his postprofessional Doctor of Physical Therapy from…
Chapters & learning objectives

1. Introduction
This chapter examines the history of shoulder arthroplasty and the demographic factors, such as advanced age and smoking, that contribute to the high prevalence of glenohumeral osteoarthritis. Clinicians will compare historical inpatient protocols to modern same-day discharge trends to better understand how changing patient expectations drive the need for early therapeutic intervention.

2. Rehabilitating the Shoulder
Clinicians will explore the essential phases of shoulder rehabilitation, emphasizing the use of manual therapy and periscapular techniques to improve functional mobility. This section highlights the importance of standardized protocols and the protection of healing tissues, such as the subscapularis, during the initial six weeks of recovery.

3. Postoperative Exercises and Expectations
This chapter provides actionable techniques for the early facilitation of movement, focusing on short-lever deltoid exercises and the “balanced position” to optimize the kinetic chain. Participants will analyze expected range-of-motion outcomes for different surgical procedures and learn to identify when patients are ready to transition from joint protection to functional strengthening.

4. Reverse Total Shoulder Arthroplasty
As the utilization of reverse shoulder arthroplasty continues to grow, therapists must master the unique biomechanics and strict dislocation precautions required for this procedure. This chapter details the long-term survival rates of modern implants and provides evidence-based guidance for safely returning patients to high-demand activities such as golf, swimming, and weightlifting.
More courses in this series

Optimizing Outcomes After Total Joint Arthroplasty
John O’Halloran
Optimizing Function After Shoulder Arthroplasty
John O’Halloran
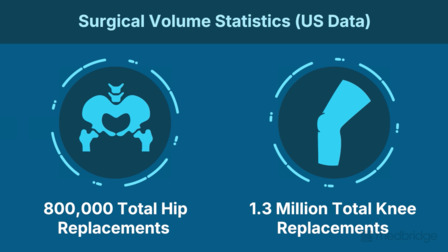
Optimizing Gait After Hip Arthroplasty
John O’Halloran
Optimizing Recovery After Knee Arthroplasty
John O’Halloran
Optimizing Complex Cases in Joint Arthroplasty
John O’Halloran