Pelvic Pain in Athletes: Does Anatomical Diagnosis Matter?
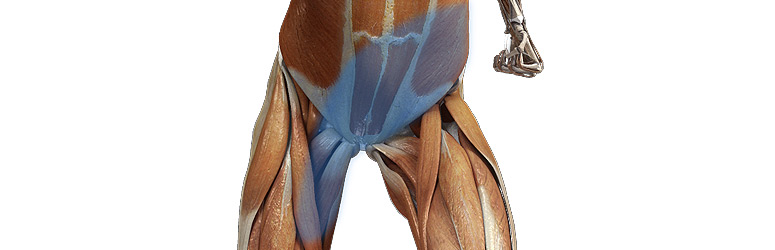
We pay attention to anatomical differentiation in every other part of the body, but it can feel like the pelvis, particularly the pelvic floor, doesn’t get the attention it deserves.
So does anatomical differentiation in the pelvis matter when treating athletic groin pain (AGP)?
Yes, and here’s why.
Navigating & Understanding AGP
The groin has been described as the Bermuda Triangle of sports injuries.1 Similar to what we see with pelvic pain generally, an anatomical dysfunction in the pelvis rarely presents in isolation – for example, the interaction in dysfunctions of the abdominal and adductor aponeuroses. Additionally, there is confusion in the terminology from athletic pubalgia to Gilmore’s Groin to osteitis pubis. Nothing is simple or straightforward when it comes to pelvic pain, especially in athletes.
AGP is defined as a chronic injury to the inguinal region (junction of the torso and lower limb). The reported incidence rate is between 3 and 23% of the physically active population.2 AGP has also ended many athletic careers.
Differential diagnosis can be challenging due to the complex anatomy of the region and the wide variety in terminologies. A recent systematic review reported 33 different terminologies used in 72 studies.6 Even the literature disagrees on the groupings of presentation subcategories beyond the broad regions of the abdominal wall, adductors, hip flexors, and pubic bone – not to mention pelvic floor dysfunction.
Assessment
To assess chronic pain in the groin, gluteal and greater trochanter triangle areas, clinicians can use an assessment method based on pathoanatomical principles.3 This approach enables clinicians to differentiate more easily between pathological conditions, target their investigation, and subsequently manage the specific diagnoses.
Recently, the research community has recognized that intra-articular hip disorders, pelvic floor, and chronic pelvic pain near the hip are closely related. For example, Coady et al suggests that vulvar pain may be generated by FAI’s effect on pelvic muscles and nerves, meaning treatment with arthroscopy may improve the resulting vulvodynia.4
Today’s sports medicine clinician, when facing the nebulous diagnosis of groin pain must, at a minimum, factor in the assessment of:
- The lumbar spine
- The pelvic girdle
- The hip
All the potential muscular components need to be assessed as well, particularly, the psoas, iliacus, rectus abdominous, the adductors, the gluteals, the hamstrings, piriformis, obturator internus and the pelvic floor muscles (ideally both externally and internally).
Case Study
Gluteal injuries, proximal hamstring injuries, and pelvic floor disorders are common among runners. The literature suggests that hip, pelvis, and/or groin injuries occur in 3.3% to 11.5% of long distance runners.5
A 2013 case study by Podschun looked at a 45-year-old female distance runner experiencing proximal hamstring pain for several months.5 The pain limited her ability to tolerate sitting and caused her to cease running. Examination of the patient’s lumbar spine, pelvis, and lower extremity led to the initial differential diagnosis of hamstring syndrome and ischiogluteal bursitis.
The patient’s primary symptoms improved during the initial four visits, which focused on education, pain management, trunk stabilization and gluteus maximus strengthening; however, the pelvic pain persisted. Further examination led to a secondary diagnosis of pelvic floor hypertonic disorder. Interventions to address the pelvic floor resolved the symptoms and the patient returned to running.
Podschun’s conclusion: “This case suggests the interdependence of lumbopelvic and lower extremity kinematics in complaints of hamstring, posterior thigh, and pelvic floor disorders. This case highlights the importance of a thorough examination as well as the need to consider a regional interdependence of the pelvic floor and the lower quarter when treating individuals with proximal hamstring pain.”5
Treating a Multifactorial Issue
Although athletic pubalgia may be the leading clinical consideration when an athlete presents with anterior pelvic pain, other dysfunctions – musculoskeletal, visceral, and gynecologic – may contribute to the pain as well. In fact, groin pain related to activity is usually multifactorial. To successfully assess and treat it, we must understand the contributions from the hip, the bony pelvis/its regional musculature, the diaphragm, the psoas, the abdominals, the adductors and, of course, the pelvic floor muscles.
- Bizzani, M, The Groin Area: The Bermuda Triangle of Sports Medicine?, Br J Sports Med 2011;45:1
- King E et al. Athletic groin pain: a systematic review and meta-analysis of surgical versus physical therapy rehabilitation outcomes. Br J Sports Med.(2015) Online First
- Falvey, E et al. The groin triangle: a patho-anatomical approach to the diagnosis of chronic groin pain in athletes. Br J Sports Med (2009) 43:213–220
- Coady et al, Vulvodynia and Concomitant Femoro-Acetabular Impingement: Long term follow up after Hip Arthroscopy Journal of Lower Genital Tract Disease • Volume 19, Number 3, July 2015
- Podschun et al. Differential Diagnosis of Deep Gluteal Pain in a Female Runner with Pelvic Involvement: A Case Report. Int J Sports Phys Ther. 2013 Aug; 8(4): 462–471.
- Weir et al. Doha agreement meeting on terminology and definitions in groin pain in athletes. Br J Sports Med (2015) 49:768-774




