SOUND Advice: Assessing Speech Sound Disorders

Nearly one in twelve children between the ages of 3 and 17 have some type of communication disorder.1 Speech sound disorders (SSDs) are the most prevalent, particularly among children aged 3 to 6 years old.2 This means that if you work with a pediatric population, you are highly likely to have children with a speech sound disorder on your caseload.
Although SSDs themselves are relatively easy to identify at the outset, you’ll also need to identify the nature and severity of the disorder and any underlying causes or contributing factors before you can determine an appropriate treatment plan.3 And because SSDs are complex and diverse neurodevelopmental disorders that range in both severity and type, assessment can be challenging.4
SSDs include articulatory, phonological, and motor speech disorders. They can co-occur with other communication impairments, such as language impairment, literacy difficulties, or fluency disorders. Given the complexity of SSDs, differential diagnosis is essential to designing effective intervention.
Assessing SSDs: Clinical Decision-Making
Assessment requires several steps, including:
- Identifying that an SSD is present
- Analyzing the errors or error patterns
- Differential diagnosis
A basic assessment battery includes:
- Hearing and speech mechanism assessment
- Developmental, educational, medical, and family case history
- Receptive, expressive, and literacy language skills assessment
- Speech skills (including single words, connected speech, and stimulability) and perception skills assessment
Once the data from these initial assessments are collected, you must decide how to analyze the child’s speech errors.
Two Analysis Frameworks with Multiple Options
The oldest and most common way to assess a child’s speech errors is SODA: Substitution, Omission, Distortion, and Addition. This articulatory approach describes the types of sound errors produced by the child. Phonological Process Analysis (PPA) is a common phonological approach that describes the error patterns in a child’s speech using phonological processes such as final consonant deletion, cluster reduction, stopping, and fronting. More recently, broad-based approaches such as Systemic Phonological Analysis of Child Speech (SPACS) incorporate more linguistic principles to describe a child’s sound system.
With so many options, how do you choose the best approach to analyze a child’s speech?
For starters, these options all fit into two frameworks: Relational Analysis and Independent Analysis.

Describing Analysis Perspectives
Within these two frameworks, we can drill down further to characterize these analysis perspectives as follows:
- Error analyses vs. descriptive analyses
- Adult-based analyses vs. child-based analyses
- Sound-based analyses vs. system-based analyses
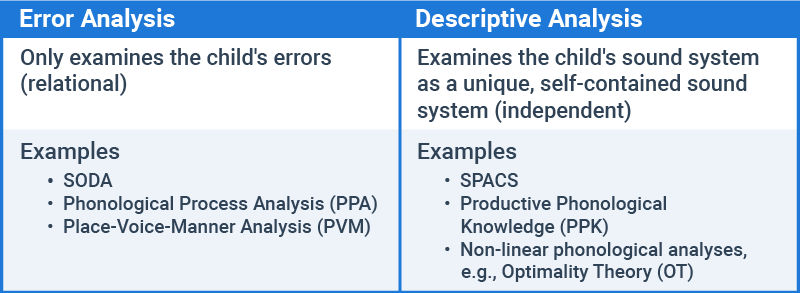
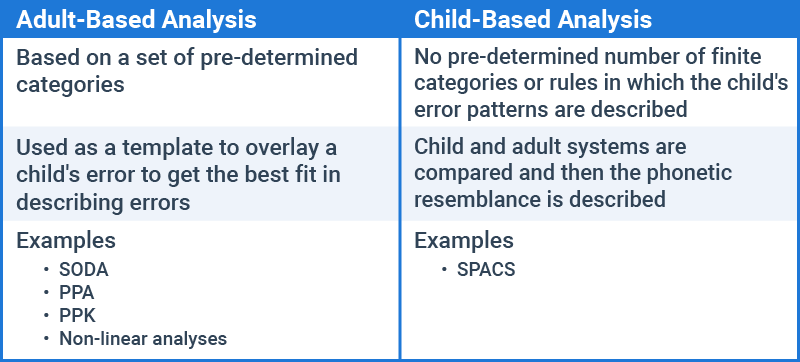

Now we can put all of this together to compare these various analyses at a glance.
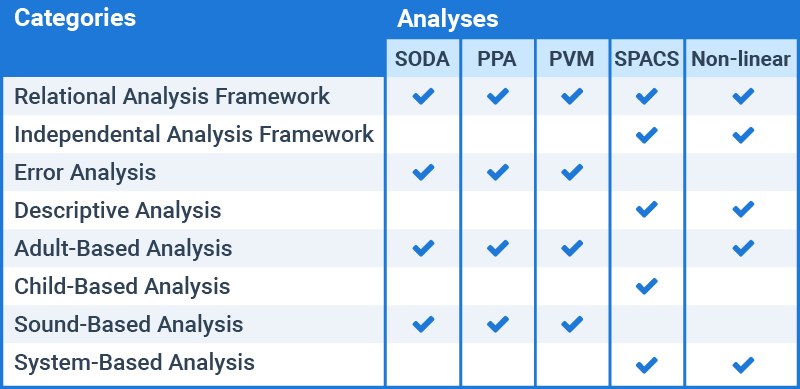
Based on this summary, you can see that SODA, PPA, and PVM have identical categorization. All three are relational, error, adult- and sound-based analyses. On the other hand, SPACS and non-linear analyses such as OT share some commonalities as they both have independent and relational qualities and are descriptive, system-based analyses. SPACS, the only child-based analysis, is unique.
One analysis approach does not fit all children, and this means that clinicians need to decide on a case-by-case basis which approach is right for a particular child. These guidelines will help you make that decision:
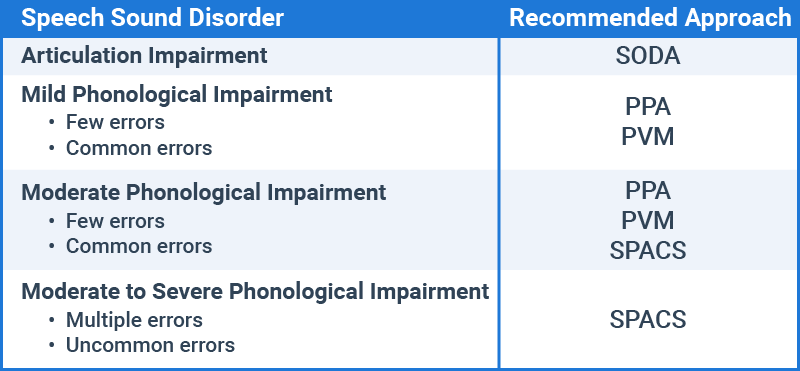
Making a Differential Diagnosis
For some children, we need to go beyond a basic assessment to make a differential diagnosis of a motor speech disorder or to differentiate learners and their skills for intervention planning. We may need to include perception testing and more in-depth stimulability testing in order to make intervention decisions related to type of approach and level of intervention, as well as make informed decisions about target selection. If a motor speech disorder is suspected, additional testing may include maximum performance tasks such as diadochokinetic rate, multisyllabic words, and non-word repetition to assess stress patterns and phonotactic constraints. We may also include cueing levels as part of a dynamic assessment to provide information for intervention planning.
SSDs are complex, diverse, and multifaceted. Assessment does not stop at a single-word test; rather, it involves sound decisions regarding how to best analyze the child’s errors and plan effective intervention. Your assessment may need to go beyond a basic assessment battery to include additional testing, such as perception, stimulability, and maximum performance tasks to make a differential diagnosis and intervention decision based on the child’s abilities in perception and stimulability.
Just because SSDs are the most common communication disorder doesn’t mean they are simple to assess. As with intervention decisions, we need to use sound clinical decision-making based on reasoned evidence-based practice to design the most appropriate and effective intervention given the characteristics of each unique child’s SSD.
- Ketelaars, M. P., Cuperus, J. M., van Daal, J., Jansonius, K., & Verhoeven, L. (2009). Screening for pragmatic language impairment: The potential of the Children’s Communication Checklist. Research in Developmental Disabilities, 30(5): 952–60.
- Shriberg, L. D., Tomblin, J. B., & McSweeny, J. L. (1999). Prevalence of speech delay in 6-year-old children and comorbidity with language impairment. Journal of Speech, Language, and Hearing Research, 42(6): 1461–81.
- Miccio, A. W. (2005). Components of phonological assessment. In A. Kamhi & K. Pollock (Eds.) Phonological Disorders in Children: Assessment and Intervention. Baltimore, MD: Brookes Publishing Co.
- Shriberg, L. D. (2010). Childhood speech sound disorders: From postbehaviorism to the postgenomic era. In R. Paul R & P. Flipsen (Eds.) Speech Sound Disorders in Children. San Diego, CA: Plural Publishing.




