Conservative Management of Trigger Finger
January 10, 2023
3 min. read

Trigger finger, also known as stenosing tenosynovitis and, in some cases, trigger thumb, is an irritating and sometimes painful condition. It occurs when the tendon sheath becomes inflamed and thickened, causing the tendon to catch on the sheath.
Over time, the tendon becomes inflamed and irritated and develops nodules. This leads to the tendon becoming stuck at the base of the finger or thumb, usually at the A1 pulley. The proximal interphalangeal joint may remain bent and need to be passively extended.
Treatment Options
Conservative treatment options for a trigger finger or trigger thumb include:
Decreasing inflammation: Instruct the patient to avoid heavy gripping or pinching.
Splinting the joint: This will prevent motion in the joint where the catching is occurring. Different splint options include:
Custom fabrication of a ring splint
Thermoplastic
Metal
Prefabricated splints
Hand therapy: This can include:
Ultrasound over the inflamed tendon and sheath to reduce inflammation and scar adhesions
Friction massage over the tendons, which may break up and decrease adhesions, nodules, and edema
Passive range of motion to the metacarpal and interphalangeal joints, followed by localized ice or ice massage
Passive intrinsic and extrinsic stretching of the hand and wrist with patients avoiding active use of the involved finger or thumb to allow the inflammation to subside
Medbridge offers a Certified Hand Therapy (CHT) Prep Program for clinicians to learn the skills above, pass the Hand Therapy Certification exam, and earn CEUs.
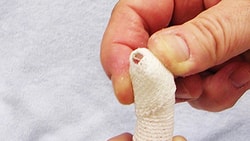
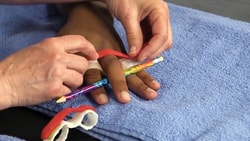
Splinting for Trigger Finger
Wearing a splint is necessary to relieve trigger finger symptoms and avoid surgery. Finding the right splint for the patient, ideally one that matches the patients aesthetic and is comfortable to wear, will help to ensure the patient will wear it as prescribed. Ring splints, for example, look like jewelry while still preventing motion and catching/triggering of the tendon and decreasing inflammation. However, ring splints can be more expensive and are generally used for chronic conditions. Examples of splints are below.
[gallery link="file" size="full" ids="12944,12942,12943"]
The patient should continue to splint the finger or thumb for six weeks or longer if the inflammation continues. Some patients may require up to six months for the condition to resolve. As pain and inflammation improve, continue with night splinting and gradually resume normal hand activities.
What to Do When Trigger Finger Symptoms and Pain Continue
If there is still pain after conservative treatment, steroid injections mixed with a numbing agent can help. The injection is placed superficial to the tendon sheath and decreases tendon sheath and tendon inflammation, resolving trigger finger symptoms.
If trigger finger symptoms continue, the next and final option is a surgical procedure called the trigger finger release.
Many patients can overcome their trigger finger without surgery if it is addressed early through conservative treatments such as splinting. Some infants and children will even outgrow this condition. However, if the finger remains bent and is stuck or contracted for too long by any patient, surgery is the only option.
You can learn more about treating trigger finger in the Medbridge course, Treatment for Five of the Most Common Upper Extremity Conditions, presented by Mike Szekeres, PhD, OT Reg (Ont.), CHT. For more information on splinting, check out the Medbridge course, Evidence-Based Intervention to Restore Dynamic Thumb Stability, presented by Virginia OBrien, OTD, OTR/L, CHT.
Below, watch Mike Szekeres discuss trigger finger treatment in this brief clip from his MedBridge course "Treatment for Five of the Most Common Upper Extremity Conditions."