Preparing for Home Health Value-Based Purchasing: What to Know and What to Expect

As part of its final rule for 2022, CMS has announced that it will expand the Home Health Value-Based Purchasing Model (HHVBP) from nine states to 50 states beginning on January 1, 2023. With the 2022 pre-implementation period in full swing, it’s important to act now to ensure your agency is ready for the new value-based model. In this article, we’ll break down the key elements of HHVBP and provide guidance on how you can best prepare your staff and organization.
What is the importance of Home Health Value-Based Purchasing?
HHVBP is a major step forward in value-based care for home health agencies, shifting reimbursement away from volume to the quality of care delivered. The pilot model that CMS rolled out in nine US states was designed to reward agencies with higher achieved or improved quality scores and reduce payments to those with lower performance scores. According to CMS, the pilot model has been highly successful, resulting in an average 4.6 percent improvement in home health agencies’ quality scores and an average annual savings of $141 million to Medicare.1 Agencies in participating states have also seen a reduced total cost of care, a reduction in unplanned hospitalizations, and improved patient function and experience, and have been satisfied with the model overall.2
CMS has designated 2022 a pre-implementation year, providing training and resources to agencies to help prepare them for success. The year 2023 will be the first performance year, and payment adjustments will begin in 2025.
How will Home Health Value-Based Purchasing affect my agency?
Starting in 2023, CMS will be implementing a 5 percent plus-or-minus rate adjustment based on the quality of care delivered (with 2023 quality scores impacting payment rates starting in 2025). Payment adjustments will be based on a set of quality measures in a given year relative to agencies that CMS considers similar to yours.
What measures are included in Home Health Value-Based Purchasing?
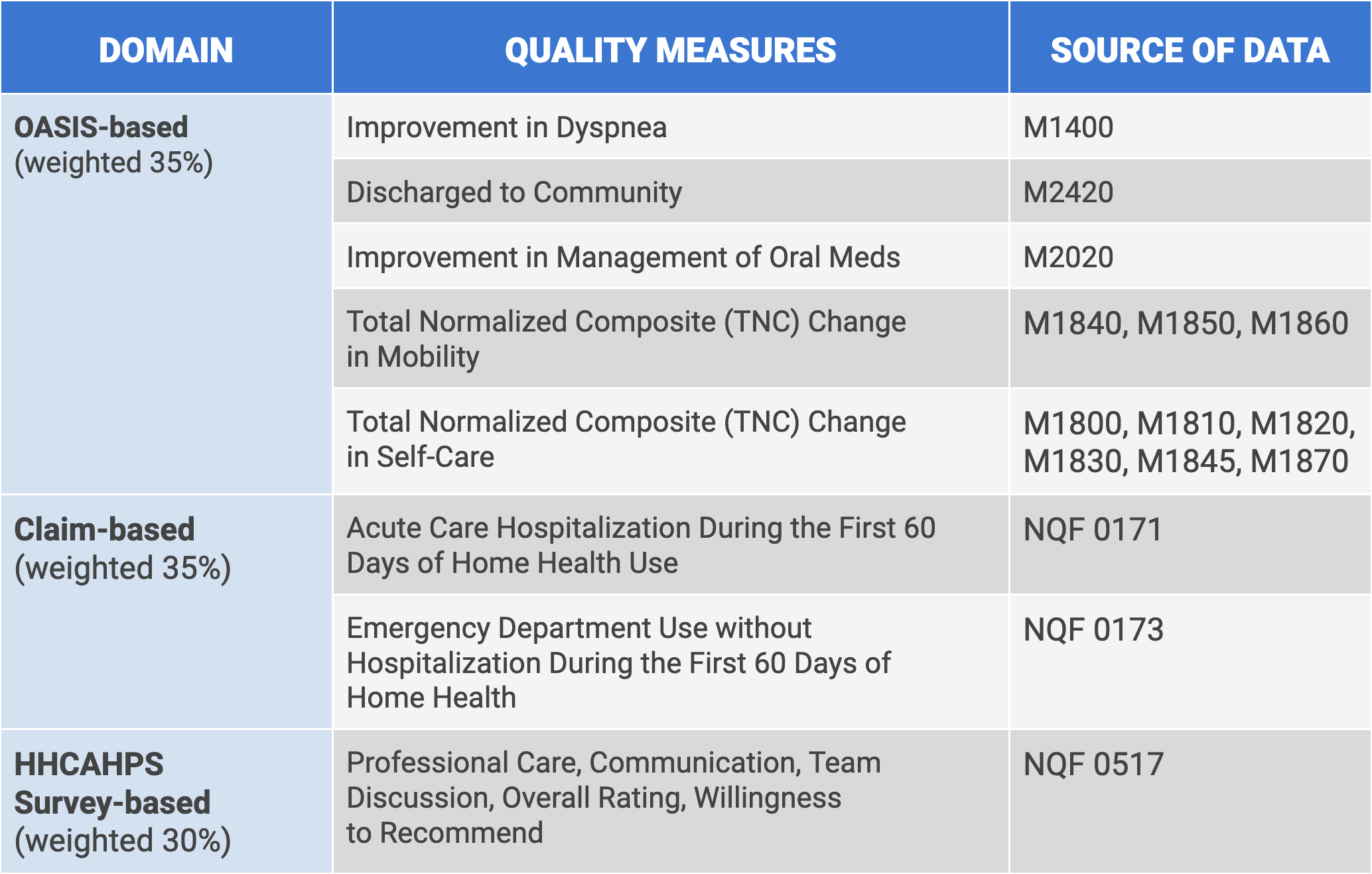
Your agency’s quality score will be determined by three main measures, weighted as follows:
- Thirty-five percent of the quality score is based on OASIS accuracy.
- An additional 35 percent of the score will be based on submitted claims for ED visits, as well as hospitalizations that occur within the first 60 days of a patient on service.
- Thirty percent of the score will be based on patient satisfaction (the HHCAHPS survey).
How can I solve for Home Health Value-Based Purchasing?
Provide targeted, efficient OASIS training.
To succeed under the HHVBP model, agencies will need to ensure accurate and complete documentation and help staff understand the impact it can have on quality measures. Providing effective onboarding and ongoing training can help your agency establish a strong foundation for accurate OASIS data collection.
Reduce readmissions with effective patient management.
Keeping patients engaged and activated between visits is key to helping them meet their treatment goals and reducing readmissions. By combining digital healthcare tools with patient education and staff training, you can replace and supplement costly in‑person visits, foster patient self-management, develop standardized care pathways, and implement best practices to keep your patients engaged and healthy.
Improve patient satisfaction.
To begin improving your HHCAHPS scores, work to build a patient-centered culture that engages and supports your patients. Train your staff on providing clear, empathetic communication alongside high-quality care, and ensure that your patients have access to evidence-based engagement and education tools that encourage them to be active partners in their care.
How can MedBridge help with Home Health Value-Based Purchasing?
The MedBridge Home Health Value-Based Purchasing Solution helps agencies prepare for the transition to HHVBP with expert-led educational resources and effective quality and engagement solutions to set your agency up for success. Agencies are leveraging it to:
Improve OASIS accuracy
Poor OASIS documentation can be costly. Reduce OASIS errors to ensure accurate outcomes and reimbursement by:
- Efficiently onboarding staff with our full-scope 10-course OASIS training series (soon to be updated for OASIS-E)
- Reinforcing training with short microlearning courses to remediate common errors
- Streamlining assignment, tracking, and reporting with an intuitive Learning Management System
Reduce readmissions
Readmissions directly impact your HHVBP scores and your reimbursement. Improve chronic condition management, reduce falls, and decrease medication errors by:
- Elevating your care team to manage complex conditions with education on CHF, COPD, diabetes, and cancer
- Improving patient self-management with effective patient education, exercises, and remote communication tools
- Preparing managers to better support clinicians with leadership and change management training
Boost HHCAHPS scores
Lagging HHCAHPS scores could lead to a drop in reimbursement—and referrals. Elevate patient satisfaction by:
- Training clinical and non-clinical staff on soft skills with targeted microlearning courses
- Establishing good patient rapport with courses focusing on communication and HHCAHPS
- Building a strong therapeutic alliance with digital engagement and communication tools
Access valuable educational resources
Our HHVBP Resource Center helps you prepare for success with expert-led webinars, guides, and articles.
1. CMS.gov, Expanded Home Health Value-Based Purchasing Model
https://innovation.cms.gov/innovation-models/expanded-home-health-value-based-purchasing-model
2. Pozniak, A., Turenne, M., Lammers, E., Mukhopadhyay, P., Slanchev, V., Doherty, J., & Green, L., et al. (2021). Evaluation of the Home Health Value-Based Purchasing (HHVBP) Model: Fourth Annual Report. Arbor Research: Ann Arbor, MI. Retrieved from https://innovation.cms.gov/data-and-reports/2021/hhvbp-fourthann-rpt.