Going Beyond Central Sensitization: A Holistic Approach to Examination & Treatment

Become an expert in orthopedics with MedBridge’s Orthopedic Excellence Certificate series. Gain evidence-based insights into assessment and treatment for the spine, upper quarter, and lower quarter to relieve patient pain and improve their quality of life.
The Pain Science Boom
Pain science research has been prolific over the last 15 years. A current search of PubMed linking the terms “pain” and “science” produces, incredibly, over 122,000 articles.
Rehabilitation professionals have especially embraced pain science, perhaps because we are the best conservative, non-pharmacologic, and holistic hope for patients with chronic pain. It seems that currently I cannot go through a day in the clinic or in the halls of academia without someone mentioning pain science. And this is a good thing!
The Oversimplification of Pain Science
Unfortunately, like many good things, pain science has been adopted but oversimplified, becoming synonymous with the term “central sensitization” (CS). Many practitioners have come to associate all pain that lasts longer than six weeks with central sensitization, and therefore, treat their patients with pain science education. Simple diagnosis, simple treatment.
3 Issues with a Simplistic Approach to Shoulder Pain
While this simplistic approach may not be a bad thing in and of itself, it’s too simple a solution for too complex a problem. Why is this?
For one thing, CS—an amplification of neural signaling within the central nervous system—exists because of pain pathway facilitation and a malfunction of descending inhibitory pathways resulting in hypersensitivity to pain.1 CS is only one of many types of pain, including, for example, neuropathic pain and peripheral sensitization.
Next, we have limited evidence of CS pain being a major factor in shoulder pathologies that cause pain. A 2015 systematic review noted that evidence was emerging but still in its infancy.2 My further review of literature when creating the MedBridge courses “Evidence-Based Examination of the Shoulder” and “Evidence-Based Treatment of the Shoulder” suggests that evidence of CS in shoulder pathologies is still in its infancy with frozen shoulder and subacromial pain being diagnoses where CS may play a part in the pain experience.
To make matters more complex, it seems that cognitive behavioral factors play an important role in the pain experience, regardless of the type of pain. These factors, which may include coping strategies, anxiety, depression, kinesiophobia, sleep disturbance, and other comorbidities, also play a role in outcomes.
Since evidence of CS in shoulder pathologies is currently scarce and we know that multiple other biopsychosocial factors are associated with pain and outcomes, I would suggest a less simple, more multi-faceted, and personalized care approach.
Enter the Pain and Disability Drivers Model
Providing personalized care requires an understanding of all the potential drivers behind the pain and disability that each patient experiences and tailoring treatment to address those psychological, social, and biological drivers.
The Pain and Disability Drivers Model (PDDM), an integral part of the new Orthopedic Excellence Series, was created to identify the primary drivers of pain and disability that are unique to each patient.3 As seen in Figure 1, the PDDM involves standardized assessment elements within five domains of pain and disability:
- Nociceptive pain drivers
- Nervous system dysfunction drivers
- Comorbidity pain and disability drivers
- Cognitive-affective drivers
- Contextual disability drivers
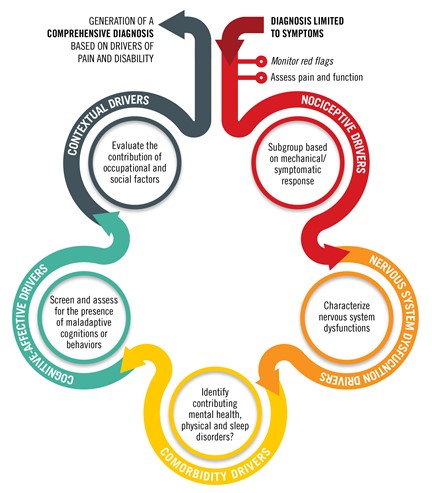
Figure 1. The Pain and Disability Drivers Model
Awareness of the multi-faceted drivers of pain and disability enables the practitioner to tailor the examination and treatment to each individual patient, providing personalized care. It is my strong belief that you will be a more complete practitioner by approaching your patients with the PDDM in mind.
- Nijs, J., Torres-Cueco, R., van Wilgen, C. P., Girbes, E. L., Struyf, F., Roussel, N., & van Oosterwijck, J., et al. (2014). Applying modern pain neuroscience in clinical practice: criteria for the classification of central sensitization pain. Pain Physician, 17(5), 447–57.
- Sanchis, M. N., Lluch, E., Nijs, J., Struyf, F., & Kangasperko, M. (2015). The role of central sensitization in shoulder pain: a systematic literature review. Seminars in Arthritis and Rheumatism, 44(6), 710–6.
- Tousignant-Laflamme, Y., Martel, M. O., Joshi, A. B., & Cook, C. E. (2017). Rehabilitation management of low back pain—it’s time to pull it all together! Journal of Pain Research, 10, 2373–2385.










